Laser Lengthens Survival, Shortens Recovery For Glioblastoma Patients
A 60-year-old Colorado woman diagnosed with glioblastoma (GBM), the most common, aggressive form of malignant brain cancer in adults, with poor life expectancy, recently came to Miami Valley Hospital for an innovative, minimally invasive surgical procedure that can increase the survival and quality of life of glioblastoma patients.
The procedure, called laser interstitial thermal therapy (LITT), was performed by Premier Health neurosurgical oncologist Andrew E. Sloan, MD, who is widely recognized for helping develop LITT and writing the paper that led to LITT gaining US Food and Drug Administration (FDA) approval. Dr. Sloan, director of the Brain Tumor program at Premier Health and Wright State University Boonshoft School of Medicine, performed the procedure on the mother of one of the Colorado patient’s friends.
The earlier patient, who also had recurrent glioblastoma, is disease-free more than five years after her surgery for the recurrence. That’s substantially longer than the average 14- to 16-month overall survival rate anticipated for GBM patients. The median survival rate for recurrent GBM that returns after a full course of treatment is typically three to five months.
How LITT Works
Due to the nature and location of the Colorado patient’s tumor, removing it through conventional surgery – a craniotomy, which requires temporary removal of a piece of the skull, then microsurgery deep in the motor strip of the brain – would have been too risky, possibly worsening her condition, Dr. Sloan explains.
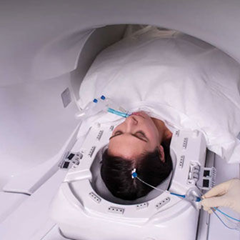
In contrast, LITT requires a very small scalp incision and tiny burr hole in the skull. A robot then guides a tiny laser fiber through and into the tumor. Then, Magnetic-resonance (MRI) directs laser energy to destroy – or ablate – the tumor.
To help plan the trajectory for the laser fiber before surgery, a preoperative MRI provides the surgical team a view of the tumor’s location in relation to critical brain structures, including motor pathways that control voluntary bodily functions.
After the procedure, patients are typically monitored overnight in the hospital and return home within 24 to 36 hours. A post-surgery MRI may be conducted to assess the ablation zone and rule out complications.
For patients with brain tumors, LITT is often part of a multidisciplinary plan that is followed by radiation therapy, chemotherapy, immunotherapy, and, in some cases, further surgery. In this case, the Colorado patient returned home for her follow-up care, but Premier Health’s multidisciplinary brain tumor team does coordinate follow-up therapy close to home for local patients.
Benefits of LITT
LITT offers patients several advantages over conventional surgery:
- Shorter hospital stays, less pain, faster recovery, and faster return to daily activities. This is due to the minimally invasive nature of LITT, featuring a tiny incision and burr hole, compared to the greater physical trauma of a conventional craniotomy.
- Access to deep or difficult lesions. Tumors located in deep brain regions or near critical structures (where open surgery carries high risk) may be more safely approached via LITT.
- Shorter time to adjuvant therapy. Because recovery is often quicker, patients can usually resume radiation or chemotherapy sooner than after a large open procedure. Radiation and/or chemotherapy can often start the next day.
- Less disruption of healthy brain tissue. Real-time magnetic resonance thermometry eliminates the need for retraction of the brain and allows precise control of the ablation zone, which can help limit damage to healthy tissue around the tumor.
- Versatility. LITT is not only used for primary brain tumors, but also for recurrent tumors, metastases (when cancer cells break away from a primary tumor), and radiation necrosis (delayed death of healthy tissue caused by radiation therapy). LITT can also be used to treat tumors in patients who are otherwise poor surgical candidates due to age or medical issues such as heart disease, diabetes, or being overweight.
In addition, emerging evidence suggests the heat from LITT may improve drug delivery or immunologic response, which is a promising potential benefit under investigation.
Multidisciplinary Brain Tumor Team
Dr. Sloan is a nationally and internationally recognized neurosurgical oncologist who helped develop LITT and helped the groundbreaking technology gain approval by the FDA. He has been a leader in advancing LITT from early feasibility to broader neurosurgical applications, especially for challenging brain tumor cases.
At Premier Health, Dr. Sloan and his colleagues have built a multidisciplinary Brain Tumor team of neurosurgeons—a neuro oncologist who provides chemo and immunotherapy for brain tumors, a radiation oncologist who specializes in radiation for brain tumors, a neuro radiologist and neuropathologist, who help interpret advanced imaging of patients and the changes in their tissue, as well as social workers, and a full clinical trial team.
The team members work together “to develop the best and most individualized treatment plan for every patient,” Dr. Sloan says.
He adds, “We recognize that not everyone is best treated with surgery, so we emphasize the importance of patient education and communication in developing truly individualized treatment plans for our patients.”
The team also works with consortiums and patient support groups, such as the American Brain Tumor Association, the National Brain Tumor Foundation, and GBM Survivors to Thrivers to find the best treatment options as close to home as possible for patients.
“Ultimately, I treat all our patients as if they're members of our own family, and I do the best for them that I can.”

Contact Us
Our specialists are ready to help you get back to the things that matter most in your life. Find a provider near you or consult our list of related practices.
Our specialists are affiliated with:

