Multiple Sclerosis: Hard Facts and Good News

Answer a few questions and we'll provide you with a list of primary care providers that best fit your needs.
When you have multiple sclerosis (MS), your immune system attacks your central nervous system. It destroys the myelin, the fatty tissue that surrounds and protects the nerve fibers of your brain and spinal cord
MS can have debilitating effects, such as paralysis, blindness, impaired thinking and loss of bladder and bowel control. That’s because scar tissue forms around the nerve fibers, preventing them from sending electrical impulses to and from your brain.
But there’s good news: The outlook for most people with MS has vastly improved over the past two decades.
“MS patients today have a very good prognosis,” says Tracy Eicher, MD, MSCS, neurologist with the Clinical Neuroscience Institute. “With early treatment and regular follow-up, we can keep most MS patients working and active and living a fairly ‘normal’ life.”
Types of MS
Dr. Eicher explains that there are four different types of MS, sometimes progressing from one to the next:
Clinically Isolated Syndrome, which is a first episode of neurologic symptoms that lasts at least 24 hours. It is caused by damage to myelin in the brain and/or spinal cord. If a second episode occurs and a brain MRI of the Spine and Brain reveals abnormal areas, it is likely you have relapsing-remitting MS.
Relapsing-Remitting MS affects about 85 percent of people with MS. They have clearly defined attacks of neurologic symptoms, which then lessen or go away for a time. The phase when symptoms go away is called remission.
Secondary Progressive MS, which, as patients age, may involve a steady decline in function rather than identifiable relapses.
Primary Progressive MS, in which people never present with clear events or relapses but show a progressive worsening of function and symptoms from the beginning.
MS Symptoms
Symptoms of MS vary from person to person, depending on the location of damaged myelin. They include:
- Blurred vision or blindness from optic nerve damage
- Muscle weakness in the arms and legs
- Problems with coordination, balance and walking
- Stiffness and spasms in muscles, called spasticity
- Fatigue
- Shaking
- Dizziness
- Numbness, prickling or pins-and-needles sensations
- Bowel and bladder problems
- Speech and hearing issues
- Impaired concentration, memory and judgment
- Depression
“The list of possible symptoms is long,” Dr. Eicher says, “because the brain is the control center for the body, and the spinal cord is the major highway through which messages pass from the brain to the body and from the body to the brain.”
The outlook for most people with MS has vastly improved over the past two decades.
Exploring Causes
In broad terms, says Dr. Eicher, the immune system causes MS. Yet, no one knows exactly why the immune system begins attacking the body.
“We have not found a specific antibody within the immune system that is the culprit,” she notes. “We know that environmental exposures play a role in triggering the immune system to seek out and attack the central nervous system, but there does not seem to be one specific thing that is the trigger. There are probably multiple variables that play a role in MS.”
Other theories are that viruses or genetic factors may contribute, although MS is not directly inherited from parent to child. Women are three times more likely than men to get the disease. MS generally appears between ages 20 and 40, but it has been known to occur even in children. Dr. Eicher says that more cases are occurring in patients over age 40, as well.
Diagnosing MS
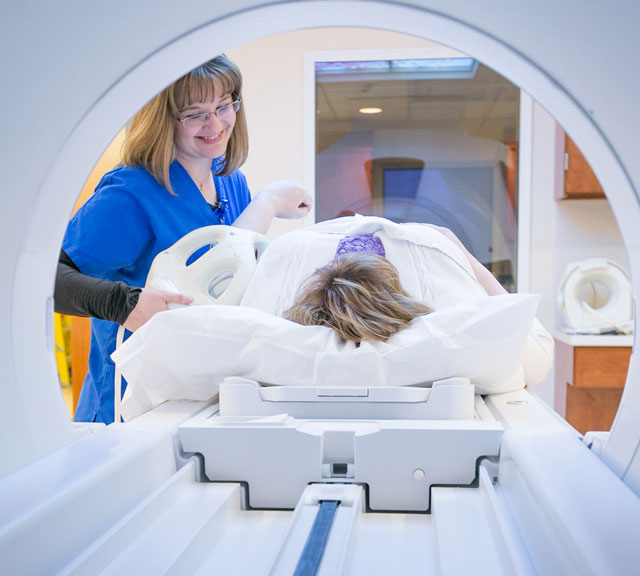
Diagnosing MS is often a matter of ruling out other conditions or diseases with similar symptoms. The starting points for identifying MS include interviewing the patient, doing a neurologic exam and getting an MRI. An MRI can reveal plaques or scarring in the brain or spine caused by MS.
Other tests include:
- Evoked potential test, which records the brain’s electrical response to auditory, visual and sensory stimuli. This test indicates if messages are moving more slowly in certain parts of the brain.
- A spinal tap, also called a lumbar puncture, can evaluate whether your spinal fluid shows abnormalities commonly seen with MS.
- Blood tests, to rule out other possible causes
Treating MS
“We have seen multiple new MS treatments come out over the past decade,” Dr. Eicher says. She adds that patients have many medication choices and promising new drugs and treatments are in development.
Your doctor can help you choose the medication that is best for you. Dr. Eicher advises that identifying the right medication requires blood tests, reviewing your medical history, including other medical conditions, your age, and “how aggressive your MS has been, where it has hit.”
She adds, “There are a lot of factors and a lot of variables to determine if you are a candidate for the available drugs, and then narrowing down what would be the best fit for your lifestyle, what will be easier for you to use, if you’ll be able to tolerate it better, and, first, if it’s safe for you.”
Some MS medications can be taken by mouth in pill form. Others require periodic injections or IV infusion administered by a health care provider. And a relatively new drug can be taken at home as a once-a-month self-administered injection using a single-use, disposable autoinjector.
The therapies vary greatly in strength, side effects, and risks. They each take a different approach to the immune system, so if one medication doesn’t work, you and your doctor can try another approach.
She adds that steroids are often given as the first treatment for a relapse. And your doctor may also treat the symptoms caused by your MS, such as spasticity or bladder issues.
A few recently approved MS drugs replace older drugs that went off patent. These older drugs have also been replaced by generics. “But that’s not always a good thing for patients,” Dr. Eicher says, explaining that the generics often require high out-of-pocket co-pays without the help of drug manufacturers’ patient assistance programs, to help you bear the cost of the drugs.
The newly approved drugs, however, are supported by patient assistance programs.
New Medications On the Horizon
Dr. Eicher is encouraged by a potential new MS treatment class that is being studied – BTK inhibitors. Three drug companies will be entering Phase 3 clinical trials of BTK inhibitor medications.
“We’re hopeful that this is going to turn out to be one of the stronger mechanisms of action to treat MS,” Dr. Eicher says. And the good thing about stronger MS drugs with a higher rate of efficacy against MS, she says, is: “They don’t necessarily have the offset of higher risk.”
What makes BTK inhibitors unique in MS treatment, she explains, is that they are better able to cross the blood-brain barrier to shut down the mechanisms in the brain that cause MS. The blood-brain barrier controls substances that can enter or leave the brain and central nervous tissue.
Most MS medications “negotiate with the immune system outside the brain, but not the immune system in the brain,” Dr. Eicher says. “We’re hopeful that BTK inhibitors – by crossing the blood-brain barrier and affecting the immune cells inside the brain and central nervous system – may be super-effective. They might even help to shut down secondary progressive — and possibly even primary progressive — MS more effectively.”
Tips for Living with MS
Dr. Eicher offers these guidelines to help you live as well as possible with MS:
- Take a positive attitude: Don't view yourself as the victim of MS. Put yourself in control by finding a neurologist you trust and can communicate with. Work with your doctor to find an MS medication that you tolerate well and that works for you.
- Take vitamin D: Vitamin D levels are important for keeping the immune system healthy. Ask your neurologist what level is right for you.
- Eat a low-sodium, low-fat diet: Too much sodium and fat are not good for MS. Fast foods or pre-packaged foods promote a more inflammatory immune system, which drives MS to be more active. Avoid processed foods and eat fresh produce and whole foods.
- Don't smoke: Nicotine worsens many MS symptoms, because it’s inflammatory for the body and the immune system. Quit smoking and avoid chewing tobacco, patches, gums or vapor with nicotine.
- Exercise: People with MS often avoid exercise. They’re afraid they will get hot and trigger a relapse. Or they think exercise will worsen their fatigue. Even if you have to make adjustments and increase activity slowly, a higher level of fitness will improve overall function. Exercise also helps improve many symptoms, including fatigue, depression, weakness and cognitive/focus issues, without medications that create potential side effects.
Answer a few questions and we'll provide you with a list of primary care providers that best fit your needs.
Source: Tracy Eicher, MD, MSCS, neurologist, Premier Health Clinical Neuroscience Institute; National Multiple Sclerosis Society; National Institute of Neurological Disorders and Stroke





