Is That Lump on My Neck a Goiter?
Answer a few questions and we'll provide you with a list of primary care providers that best fit your needs.
A goiter is an abnormal enlargement of the thyroid, the butterfly-shaped gland positioned at the front of the neck, just below the Adam’s apple. When a goiter forms, it appears as a swelling in that area. To understand what causes goiters, and how they’re diagnosed and treated, it’s helpful to know something about the thyroid itself, what its job is, and how things can sometimes go wrong.
How Does the Thyroid Work?
The thyroid distributes thyroid hormone throughout the body via the bloodstream. This hormone is important in human metabolism. It helps regulate how your body uses food for energy, and helps your brain, heart and other organs work well. The thyroid creates thyroid hormone by concentrating iodine gathered from the blood.
What Are the Most Common Causes of Goiter?
Though goiters can be caused by many things, including genetic defects, injury, infection and tumors, here are some of the most common.
- Iodine deficiency: Remember that the thyroid creates its hormone from iodine. If there’s an iodine shortage in the body, the thyroid won’t have the raw material it needs to do its job. When this happens, the brain’s pituitary gland — the body’s hormonal control center — senses the shortage of thyroid hormone. It sends a special chemical message to the thyroid gland, stimulating the creation of hormone and causing enlargement of the thyroid. Goiters caused by iodine deficiency are not common in the U.S., where iodine is added during the processing of salt and other foods.
- Hashimoto’s thyroiditis: A more common cause of goiter in the U.S., Hashimoto’s thyroiditis is a condition in which the immune system damages the thyroid and prevents it from making enough thyroid hormone. Again, the pituitary gland, sensing the situation, stimulates the thyroid to get busy making its hormone, and this stimulation can cause a goiter to grow.
- Grave’s disease: Unlike iodine deficiency and Hashimoto’s thyroiditis, which result from the production of too little thyroid hormone, Grave’s disease, an immune disorder, causes the thyroid to produce too much hormone, enlarging the thyroid gland and creating a goiter.
- Multinodular goiters: These goiters result from nodules, or lumps, that can arise on one or both sides of the thyroid, causing the gland to enlarge. They are not necessarily associated with either an increase or decrease in thyroid hormone production.
What Are the Risk Factors for Goiters?
Several factors can increase your risk of developing a goiter: being female, being over 40 years old, and being pregnant or in menopause. Additional factors include having a family history of autoimmune disease or goiter, exposure to radiation as a child or having radiation treatment of your neck or chest, and not getting enough iodine in your diet. It’s also possible that some medicines could increase the risk of goiter.
How Are Goiters Diagnosed?

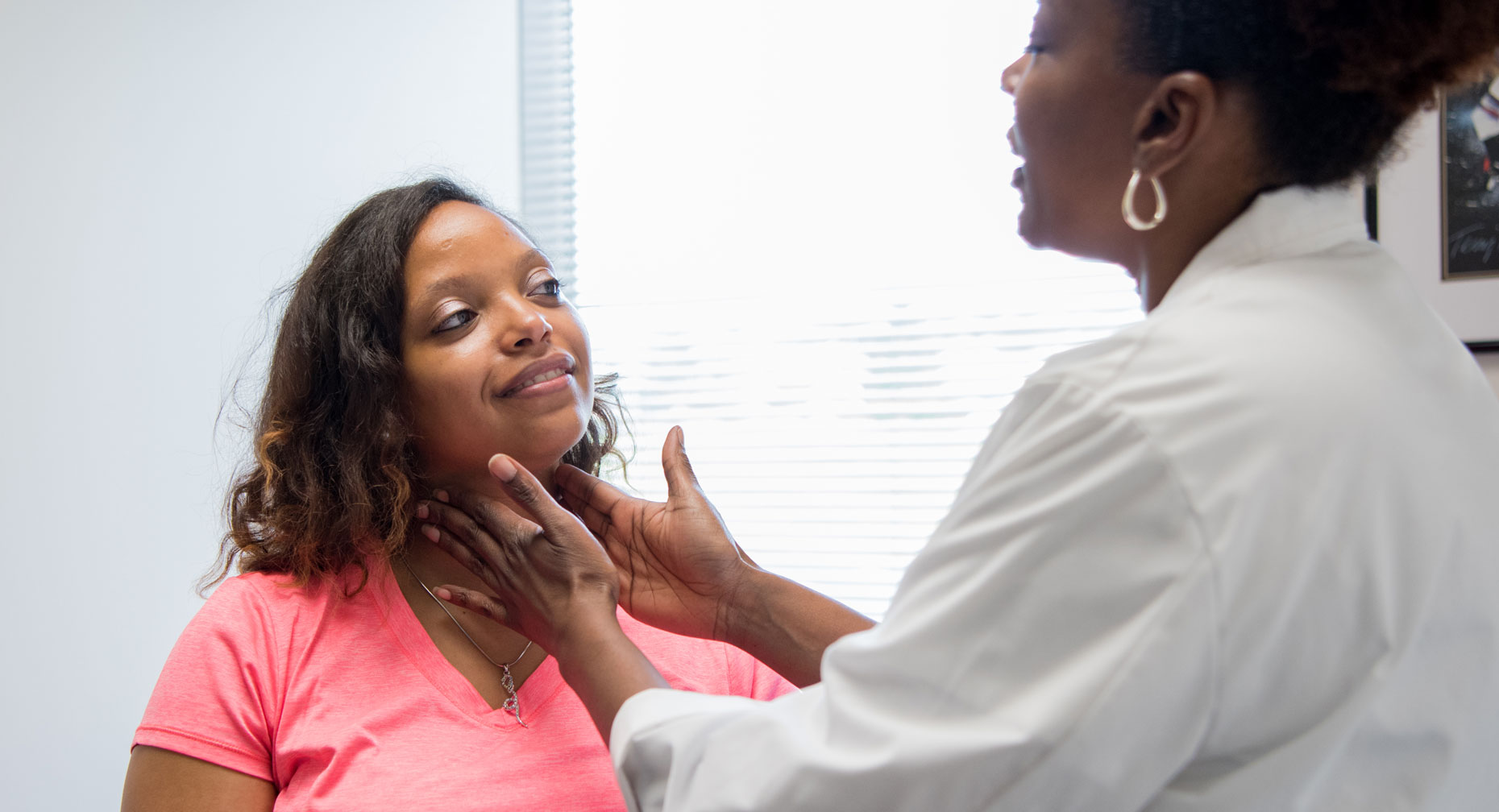
Goiters are typically discovered during a physical exam, when the doctor notices swelling in the patient’s neck. After a goiter is found, tests are done to determine whether the thyroid is producing too much or too little hormone and to pinpoint the cause. Further tests may include blood work, a thyroid ultrasound, a radioactive iodine scan, and a biopsy (on a sample of the thyroid taken with a small needle).
How Are Goiters Treated?
Treatment options depend on the cause of the goiter.
- A goiter caused by an iodine deficiency is usually treated by giving iodine supplements by mouth.
- Hashimoto’s thyroiditis is treated with a daily thyroid hormone supplement in the form of a pill.
- In the case of Grave’s disease — when the thyroid is produces too much hormone — treatment can include antithyroid drugs, radioactive iodine and surgery.
- Some goiters, such as multinodular goiters, may not be associated with abnormally high or low levels of thyroid hormone. In many such cases, no specific treatment is recommended, but if the expanding gland threatens to interfere with breathing, doctors may suggest it be removed surgically.
Most goiters can be treated with success. In some cases, however, while the goiter’s size can be reduced and thyroid hormone levels returned to normal, the goiter may not go away entirely. If you’ve been treated for a goiter, you should return to your doctor for an annual checkup.
Answer a few questions and we'll provide you with a list of primary care providers that best fit your needs.
Source: Hormone Health Network; American Thyroid Association




