Diabetes And Depression: Are They Linked?

Answer a few questions and we'll provide you with a list of primary care providers that best fit your needs.
Does diabetes cause depression? Or does depression lead to diabetes? Or is it a little bit of both?
Depression is twice as common in people with type 1 or type 2 diabetes as in the general population, according to the American Diabetes Association. Researchers aren’t yet sure why that is, but they do have some ideas.
Does One Cause the Other?
Some studies suggest that depression and type 2 diabetes share some biological origins, but more research remains to be done.
Otherwise, the connection between depression and type 1 or type 2 diabetes remains a bit of a “which came first – the chicken or the egg” type of argument. On one hand, chronic depression can lead to poor health habits (overeating, lack of exercise) that can put you at risk for diabetes. But on the other hand, a chronic illness like diabetes – with its strict dietary limits, constant blood sugar monitoring and anxiety about the future of your health – can cause stress and even trigger depression.
There are no easy answers, except to acknowledge that there does seem to be a relationship between the two diseases. However, one thing is for sure – knowing the signs of both can help you to lessen their impact.
Depression is twice as common in people with type 1 or type 2 diabetes as in the general population, according to the American Diabetes Association.
Identifying Depression
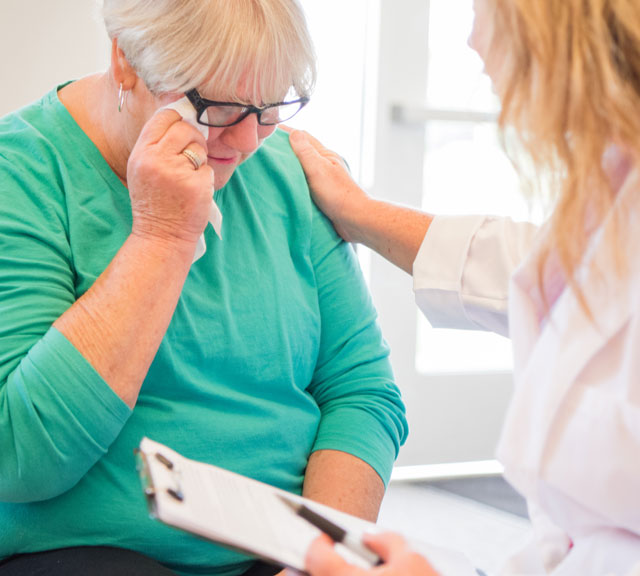
Depression is more than feeling down in the dumps. If you’ve been feeling really sad or stressed, check for these other symptoms as well:
- Loss of pleasure. You lose interest in doing things you used to enjoy.
- Change in sleep habits. You sleep more or less than usual, you have trouble falling asleep, or you wake frequently at night. Or, you wake up earlier than usual and can’t fall back to sleep.
- Change in appetite. You eat more or less than usual.
- Trouble focusing. You can't watch a TV program or read an article, or have trouble completing your work, because other thoughts or feelings get in the way.
- Loss of energy. You’re tired all the time.
- Nervousness. You can’t sit still or feel jittery because you’re anxious.
- Guilt. You feel that you can "never do anything right" and worry that you are a burden to others.
- Morning sadness. You feel more depressed in the morning than you do the rest of the day.
- Thoughts of suicide. You want to die, or are thinking about ways to hurt yourself.
If you have three or more of these symptoms, or if you have just one or two but have been feeling bad for two weeks or more, it's time to get help. Call your doctor. In particular, if you are feeling suicidal, get help immediately.
Diabetes: A Depression Copycat?
Surprisingly, some symptoms of diabetes can mimic the signs of depression. Blood sugar highs and lows can cause fatigue, overeating, irritability, anxiety, and sleep problems.
Again, talk to your doctor. He will help you sort through the symptoms and determine whether they’re linked to diabetes or indicate that you have depression. If it’s the latter, he’ll most likely refer you to a psychiatrist, psychologist, psychiatric nurse, licensed clinical social worker, or professional counselor for help.
Coping With Diabetes And Depression
Many of the same things that help control blood sugar are helpful in managing depression. This includes eating a healthy diet, exercising, and finding ways to reduce your stress.
Coping with chronic illness is challenging. However, changing your lifestyle, working with your physician, and enlisting the help of a mental health professional will go a long way in helping you feel your best regardless of your diagnosis.
Answer a few questions and we'll provide you with a list of primary care providers that best fit your needs.
Source: American Diabetes Association; National Institute of Mental Health; Dr. Joseph Allen; Premier Health Family Care of Vandalia